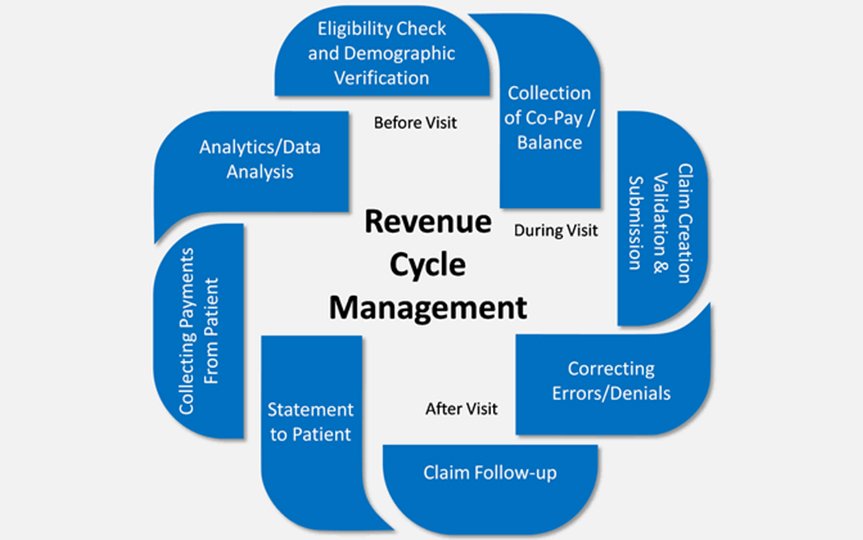
Healthcare finance is changing faster than ever. Between shifting payer rules, evolving technology, and tighter margins, staying ahead matters. Revenue cycle management services have moved well beyond basic billing.
In 2026, they are reshaping how healthcare organizations run financially.
Here is what is driving the change and what it means for your practice.
Automation Is Taking Over Repetitive Tasks
Manual processes slow everything down. Eligibility checks, claim scrubbing, and prior authorization requests used to require significant staff time. Now, automation handles much of it in the background.
Practices using automated RCM workflows are seeing faster claims processing and fewer human errors. Staff can focus on exceptions and patient-facing work instead of routine data entry. This shift is becoming standard, not optional.
RCM Services for Hospitals Are Going More Predictive
Large health systems are moving from reactive to predictive revenue cycle management. Rather than fixing denials after they happen, the goal is to prevent them entirely.
RCM services for hospitals now include denial prediction tools that flag high-risk claims before submission. Analytics also help identify which payers and procedures carry the highest denial rates so that billing teams can prepare accordingly.
Patient Financial Experience Is Getting More Attention
Patients are paying more out of pocket than ever. High-deductible plans are now common, and patients expect transparency about their financial responsibility before receiving care.
Forward-thinking RCM service providers are building better patient communication into their workflows. This includes upfront cost estimates, flexible payment options, and clear billing statements. Practices that prioritize this are seeing better collection rates and higher patient satisfaction.
What RCM Service Providers Are Doing Differently in 2026
The best RCM service providers today are not just processing claims. They are offering performance-driven partnerships with reporting, benchmarking, and ongoing optimization.
Real-time dashboards let practice managers see where revenue is at any moment. Detailed denial analysis helps identify root causes, not just symptoms. This level of visibility was rare just a few years ago.
AI-Powered Coding Is Gaining Ground
Artificial intelligence is playing a larger role in coding accuracy. AI-assisted tools can review clinical documentation and suggest appropriate codes, reducing the time coders spend per chart.
This does not replace human expertise. It adds another layer of checks that catches errors before claims are submitted. Practices using this approach are reporting measurable improvements in clean claim rates.
Interoperability Is Improving Data Flow
One of the persistent challenges in revenue cycle management has been disconnected systems. EHRs, billing platforms, and payer portals often do not talk to each other well.
In 2026, interoperability standards are improving that connection. Better data flow means fewer keying errors, faster eligibility verification, and more accurate claims. The administrative burden on staff decreases noticeably when systems work together.
Conclusion
The revenue cycle is no longer just about billing. It is about using the right tools, the right data, and the right partners to protect and grow your practice’s revenue.
At CNC Medical Billing, we stay ahead of these shifts so our clients do not have to. Whether you are looking to modernize your processes or close persistent revenue gaps, we are built for exactly that.
Want to see what a modern revenue cycle strategy looks like for your practice? Reach out today.
FAQs
What is revenue cycle management in healthcare?
Revenue cycle management covers every step from patient registration to final payment. It includes coding, billing, claim submission, denial management, and collections.
Why is RCM important for hospitals?
Hospitals deal with high claim volumes and complex payer contracts. Effective RCM reduces denials, speeds up payments, and keeps the organization financially stable.
How has technology changed revenue cycle management?
Automation, AI-assisted coding, and predictive analytics have reduced manual work, improved accuracy, and given practices better visibility into their financial performance.
What should I look for in an RCM service provider?
Look for transparency, specialty experience, denial management capabilities, and real-time reporting. A good partner improves outcomes, not just processes.
Can small practices benefit from RCM services?
Absolutely. Smaller practices often have the most to gain because they lack dedicated billing staff and tend to leave more revenue uncollected.